Conjunctivitis
Conjunctivitis is a common eye condition that affects children, especially under 5 years of age. It can either be caused by an infection or by an allergy. Infectious conjunctivitis is contagious and may spread to other household members. Allergic conjunctivitis is more common in children with allergies such as hay fever.
Related topics sticky eye (babies under 3 months)
- a red or pink eye (or both eyes)
- redness behind the eyelid
- swelling of the eyelids, making them appear puffy
- excessive tears
- a yellow-green discharge from the eye which dries when your child sleeps, causing crusting around the eyelids
- a gritty feeling (like there is sand in the eye)
- itchiness of the eyes and eye rubbing
- children with allergic conjunctivitis almost always rub their eyes excessively. They may also have an itchy or runny nose and sneezing
Your child does not need to be excluded from school or childcare if they have conjunctivitis.
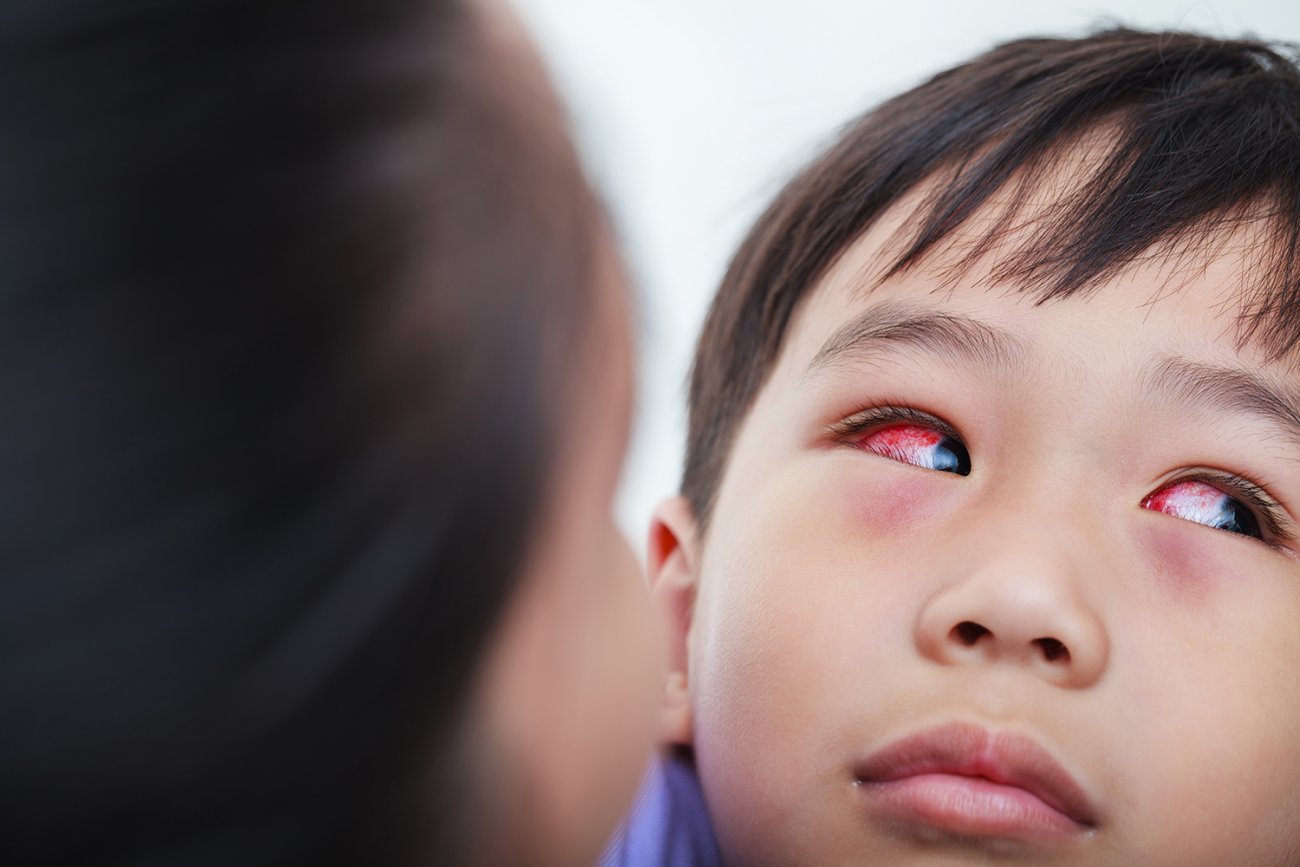
- a red or pink eye (or both eyes)
- redness behind the eyelid
- swelling of the eyelids, making them appear puffy
- excessive tears
- a yellow-green discharge from the eye which dries when your child sleeps, causing crusting around the eyelids
- a gritty feeling (like there is sand in the eye)
- itchiness of the eyes and eye rubbing
- children with allergic conjunctivitis almost always rub their eyes excessively. They may also have an itchy or runny nose and sneezing
Your child does not need to be excluded from school or childcare if they have conjunctivitis.

If your child has any of the following:
- Eyeball is bulging out
- Vision loss
- Severe pain in eyes
- Breathing very fast or breathing that stops or pauses
- Working hard to breathe, drawing in of the muscles below the rib, unable to talk or noisy breathing (grunting)
- Becomes pale, blue, mottled and/or unusually cold to touch
- Difficult to wake up, very sleepy or confused
- Weak, high-pitched, continuous cry or extremely agitated
- Has a fit (seizure)
- A temperature less than 36oC or temperature 38oC or more if baby is less than 3 months
- Develops a rash that does not disappear with pressure and seems unwell (see the 'Glass Test')
You need urgent help
Go to the nearest Hospital Emergency (A&E) Department or phone 999
If your child has any of the following:
- Red swollen eye
- Changes in vision (blurred or very sensitive to light)
- Severe headache
- Persistent vomiting
- Blisters develop on the skin next to the eye
- Babies under 1 month with a red eye(s) and yellow/green discharge
- Breathing a bit faster than normal or working a bit harder to breathe
- Dry skin, lips, tongue or looking pale
- Not had a wee or wet nappy in last 12 hours
- Sleepy or not responding normally
- Crying and unsettled
- Poor feeding (babies) or not drinking (children)
- A temperature 39oC or above in babies 3-6 months
- Temperature of 38oC or above for more than 5 days or shivering with fever (rigors)
- Getting worse or you are worried about them
You need to contact a doctor or nurse today
Please ring your GP surgery or call NHS 111 - dial 111
If your child has none of the above
Watch them closely for any change and look out for any red or amber symptoms
Additional advice is also available for families for help cope with crying in otherwise well babies
Self care
Continue providing your child’s care at home. If you are still concerned about your child, call NHS 111 – dial 111
This guidance has been reviewed and adapted by healthcare professionals across North East and North Cumbria with consent from the Hampshire development groups.
What should you do?
If your child has mild conjunctivitis, gentle cleaning of the eyes with cotton balls soaked in warm water may help your child feel better.
Clean in one direction only, outwards from the inside (nose side) of the eye. This prevents the other eye becoming infected if only one eye is affected.
Do not try to clean inside the eyelids as this may cause damage to the inside of the eye. Lubricating eye drops such as ‘artificial tears’ may give some relief.
Although infective conjunctivitis is contagious, the likelihood of it spreading is not high unless there is close contact with others. To reduce the risk of spread, they should wash their hands regularly (especially after rubbing their eyes) and avoid sharing towels, pillows, eye drops, make-up with others until the discharge from their eyes has cleared. Most children with conjunctivitis do not need treatment with oral antibiotics or antibiotic eye drops, irrespective of whether their infection is caused by a virus or bacteria.
Sore, inflamed and itchy eyes due to allergic conjunctivitis may be helped by antihistamines. Speak to pharmacist about antihistamine use for your child.
How long will your child's symptoms last?
Most conjunctivitis in children (bacterial or viral) is mild. It usually clears within 7 to 10 days without antibiotics.
Where should you seek help?
- If it is non-urgent, speak to your local pharmacist or health visitor.
- Follow the guidance in the red, amber and green boxes above
Where should you seek help?
- If it is non-urgent, speak to your local pharmacist or health visitor.
- If your child has any of the above features, urgently see your GP. For an urgent out-of-hours GP appointment, call NHS 111.
- You should only call 999 or go to your nearest A&E department in critical or life threatening situations.
Pharmacists are experts in many aspects of healthcare and can offer advice on a wide range of long-term conditions and common illnesses such as coughs, colds and stomach upsets. You don’t need an appointment and many have private consultation areas, so they are a good first port of call. Your pharmacist will say if you need further medical attention.
Sound advice
- Visit a pharmacy if your child is ill, but does not need to see a GP.
- Remember that if your child's condition gets worse, you should seek further medical advice immediately.
- Help your child to understand - watch this video with them about going to the pharmacy.
For information on common childhood illnesses go to What is wrong with my child?
Pharmacists are experts in many aspects of healthcare and can offer advice on a wide range of long-term conditions and common illnesses such as coughs, colds and stomach upsets. You don’t need an appointment and many have private consultation areas, so they are a good first port of call. Your pharmacist will say if you need further medical attention.
Sound advice
- Visit a pharmacy if your child is ill, but does not need to see a GP.
- Remember that if your child's condition gets worse, you should seek further medical advice immediately.
- Help your child to understand - watch this video with them about going to the pharmacy.
For information on common childhood illnesses go to What is wrong with my child?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns or to the Community Paediatricians or to the child and adolescent mental health services.
Contact them by phoning your Health Visitor Team or local Children’s Centre.
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information watch the video: What does a health visitor do?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns or to the Community Paediatricians or to the child and adolescent mental health services.
Contact them by phoning your Health Visitor Team or local Children’s Centre.
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information watch the video: What does a health visitor do?
Midwives provide advice, care and support for women and their babies during pregnancy, labour and the early postnatal period. They provide health education and parenting advice until care is transferred to a health visitor. This usually happens when your baby is about 2 weeks old.
Sound Advice
A midwife is an expert in normal pregnancy and birth.
Midwives provide advice, care and support for women and their babies during pregnancy, labour and the early postnatal period. They provide health education and parenting advice until care is transferred to a health visitor. This usually happens when your baby is about 2 weeks old.
Sound Advice
A midwife is an expert in normal pregnancy and birth.
GPs assess, treat and manage a whole range of health problems. They also provide health education, give vaccinations and carry out simple surgical procedures. Your GP will arrange a referral to a hospital specialist should you need it.
Sound advice
You have a choice of service:
- Doctors/GPs can treat many illnesses that do not warrant a visit to A&E.
- Help your child to understand – watch this video with them about visiting the GP or going to a walk in centre
For information on common childhood illnesses go to What is wrong with my child?
GPs assess, treat and manage a whole range of health problems. They also provide health education, give vaccinations and carry out simple surgical procedures. Your GP will arrange a referral to a hospital specialist should you need it.
Sound advice
You have a choice of service:
- Doctors/GPs can treat many illnesses that do not warrant a visit to A&E.
- Help your child to understand – watch this video with them about visiting the GP or going to a walk in centre
For information on common childhood illnesses go to What is wrong with my child?
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
A&E departments provide vital care for life-threatening emergencies, such as loss of consciousness, suspected heart attacks, breathing difficulties, or severe bleeding that cannot be stopped. If you’re not sure it’s an emergency, call 111 for advice.
Sound advice
A&E departments provide vital care for life-threatening emergencies, such as loss of consciousness, suspected heart attacks, breathing difficulties, or severe bleeding that cannot be stopped. If you’re not sure it’s an emergency, call 111 for advice.
Sound advice
School nurses care for children and young people, aged 5-19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and/or emotional health needs.
Contacting the School Nurse
Primary and secondary schools have an allocated school nurse – telephone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:-
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
School nurses care for children and young people, aged 5-19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and/or emotional health needs.
Contacting the School Nurse
Primary and secondary schools have an allocated school nurse – telephone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:-
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.



