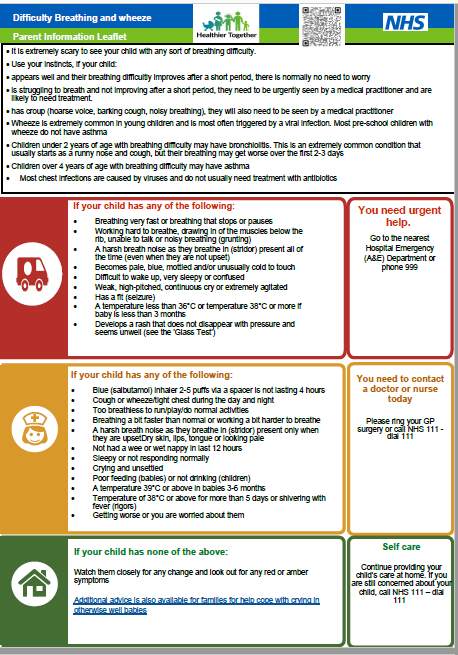
Breathing difficulties and wheeze
Wheeze is extremely common in young children. It is most often triggered by a viral infection. Most preschool children with wheeze do not have asthma.
-
Children under 2 years of age with breathing difficulty may have bronchiolitis. This is an extremely common condition. It usually starts with a runny nose and cough, but their breathing may get worse over the next 2 to 3 days. For those under 1 year of age, inhalers generally do not help.
-
If your child has croup (hoarse voice, barking cough, noisy breathing), they are likely to need assessment by a medical practitioner.
-
If you already have a salbutamol (blue) inhaler, please follow your treatment plan.
-
If your child has been diagnosed with asthma, please see our resources for how to manage asthma attacks.
If your child has any of the following:
- Breathing very fast, too breathless to talk, eat or drink
- Working hard to breathe, drawing in of the muscles below the rib, or noisy breathing (grunting)
-
Breathing that stops or pauses
- A harsh noise as they breathe in (stridor) present all of the time (even when they are not upset)
-
Is pale, blue, mottled or feels unusually cold to touch
-
Difficult to wake up, very sleepy or confused
-
Weak, high-pitched cry or can’t be settled
-
Has a fit (seizure)
-
Has a rash that does not go away with pressure (the 'Glass Test')
-
Is under 3 months old with temperature more than 38°C or under 36°C (unless fever in the 48 hours following vaccinations and no other red features)
You need urgent help.
Go to the nearest Hospital Emergency (A&E) Department or phone 999
If your child has a salbutamol (blue) inhaler please follow your treatment plan
If your child has any of the following:
-
Breathing a bit faster than normal or working a bit harder to breathe
-
A harsh noise as they breathe in (stridor) only when upset
-
Dry skin, lips or tongue
-
Not had a wee or wet nappy in last 8 hours
-
Poor feeding in babies (less than half of their usual amount)
-
Irritable (Unable to settle them with toys, TV, food or hugs even after their fever has come down)
-
Getting worse or you are worried about them
-
Is 3 to 6 months old with temperature 39°C or above (unless fever in the 48 hours following vaccinations and no other red or amber features)
-
Temperature of 38°C or above for more than 5 days or shivering with fever (rigors)
-
Temperature less than 36°C in those over 3 months
You need to contact a doctor or nurse today.
If your child has a salbutamol (blue) inhaler please follow your treatment plan
If symptoms persist for 4 hours or more and you have not been able to speak to either a member of staff from your GP practice or to NHS 111 staff, recheck that your child has not developed any red features
If your child has none of the above
-
Watch them closely for any change and look out for any red or amber symptoms
-
If your child has any other symptoms associated with their fever, you may want to look at the information on sore throat, cough, earache, diarrhoea and vomiting or tummy ache or our other pathways.
Self care
Continue providing your child’s care at home. If you are still concerned about your child, call NHS 111 – dial 111
This guidance has been reviewed and adapted by healthcare professionals across North East and North Cumbria with consent from the Hampshire development groups.
Choose appropriate sized spacer with mask (or mouthpiece if child is over 3 years with good technique and is not significantly short of breath).
-
Shake the inhaler well and remove cap.
-
Fit the inhaler into the opening at the end of the spacer.
-
Place mask over the child’s face or mouthpiece in their mouth ensuring a good seal
-
Press the inhaler once and allow the child to take 5 slow breaths between each dose or count to 10
-
Remove the inhaler and shake between every puff. Wait 1 minute between puffs.
Repeat steps 1 – 5 for subsequent doses
Plastic spacers should be washed before 1st use and every month as per manufacturer’s guidelines

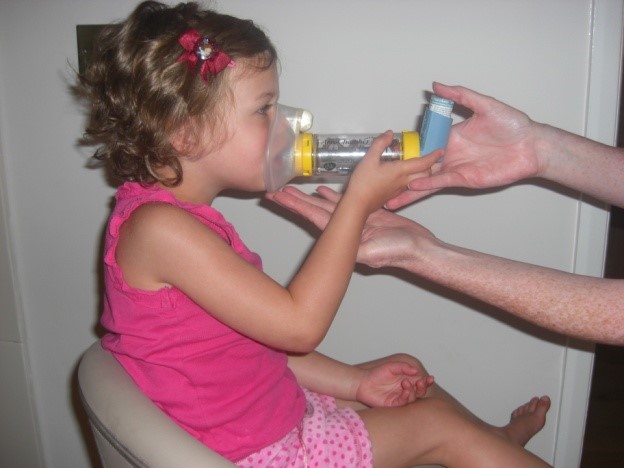

Choose appropriate sized spacer with mask (or mouthpiece if child is over 3 years with good technique and is not significantly short of breath).
-
Shake the inhaler well and remove cap.
-
Fit the inhaler into the opening at the end of the spacer.
-
Place mask over the child’s face or mouthpiece in their mouth ensuring a good seal
-
Press the inhaler once and allow the child to take 5 slow breaths between each dose or count to 10
-
Remove the inhaler and shake between every puff. Wait 1 minute between puffs.
Repeat steps 1 – 5 for subsequent doses
Plastic spacers should be washed before 1st use and every month as per manufacturer’s guidelines


-
Coughs and colds can continue for weeks before they get better.
-
Over the winter, children are likely to get one viral infection after another, which can make you think that they are never well. Things will get better in the summer months.
-
Having a cough for 2 or 3 weeks does not mean that your child needs antibiotics.
-
Children under 2 years of age with breathing difficulty may have bronchiolitis. This is a common condition that usually starts as a runny nose and cough, but their breathing may get worse over the next 2-3 days.

-
If your child has noisy breathing, they might have croup.




