Cellulitis is an infection of the deeper layers of skin. Most cases can be treated with antibiotics at home, although sometimes it needs to be treated in hospital. It can be serious if not treated quickly. It can occur at any age.
Cellulitis PIL
Symptoms of Cellulitis
Cellulitis causes an area of skin to suddenly become:
- Red
- Hot
- Swollen
- Painful
- Tender
There may also be a break in the skin, although this is not always obvious, and pus or blood-filled blisters. Your child can also have swollen painful glands.
Additional symptoms
Cellulitis can also cause extra symptoms that may develop before or alongside the changes to your skin.
These can include:
- Feeling generally unwell
- Feeling sick
- Shivering
- Chills
Occasionally the infection can spread to other parts of the body such as deep layers of tissue, blood, muscle and bone. It is important to get help quickly if you are worried.
Any part of the body can be affected. The commonly affected areas include lower legs, feet, arms, or hands, and sometimes the face particularly around the eyes. See your GP or visit your nearest minor injuries unit as soon as possible if an area of your skin turns red, painful, or hot.
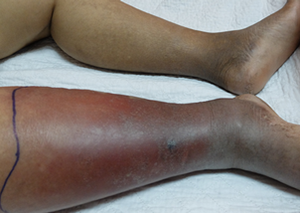
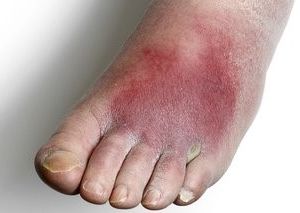
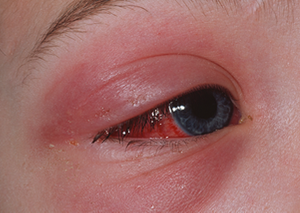
If your child has any of the following:
- Orbital (of the eye) cellulitis
- Painful or restricted eye movement
- Unable to see properly
- Eye bulging or severe headache
- A temperature less than 36oC or temperature 38oC or more if baby is less than 3 months
- Breathing very fast or breathing that stops or pauses
- Working hard to breathe, drawing in of the muscles below the rib, unable to talk or noisy breathing (grunting)
- Becomes pale, blue, mottled and/or unusually cold to touch
- Difficult to wake up, very sleepy or confused
- Weak, high-pitched, continuous cry or extremely agitated
- Has a fit (seizure)
- Develops a rash that does not disappear with pressure and seems unwell (see the 'Glass Test')
You need urgent help.
Go to the nearest Hospital Emergency (A&E) Department or phone 999
If your child has any of the following:
- Face or the area around the eye is affected
- Increasing pain or tenderness
- Worsening/spreading red area
- A temperature 39oC or above in babies 3-6 months
- Temperature of 38oC or above for more than 5 days or shivering with fever (rigors)
- Breathing a bit faster than normal or working a bit harder to breathe
- Swelling of a limb or joint
- Too painful for your child to stand
- Complaining of severe pain that is not improving with painkillers
- Dry skin, lips, tongue or looking pale
- Not had a wee or wet nappy in last 12 hours
- Sleepy or not responding normally
- Crying and unsettled
- Poor feeding (babies) or not drinking (children)
- Getting worse or you are worried about them
You need to contact a doctor or nurse today.
Please ring your GP surgery or call NHS 111 - dial 111
Self care
Continue providing your child’s care at home. If you are still concerned about your child, call NHS 111 – dial 111
This guidance has been reviewed and adapted by healthcare professionals across North East and North Cumbria with consent from the Hampshire development groups.
Causes of cellulitis
The bacteria that cause it often live harmlessly on the skin, but they can lead to an infection if they get into a break in your skin, such as:
- A bruise, cut or graze
- An animal bite or insect bite
- A leg ulcer
- Dry, cracked skin – for example, because of eczema or athlete's foot
In most cases the trigger for the infection is unknown.
The infection isn't normally spread from person to person.
Treatment
Cellulitis is usually treated with antibiotics at home. Most children will make a full recovery.
Your child will usually be given a course of treatment, and symptoms should start to improve after a few days.
Make sure to complete the whole course of medicine you've been given, even if your child is feeling better. Contact your GP if symptoms get worse after a few days or don't improve within a week.
For serious infections, treatment is usually started in hospital. Your child will be given antibiotics directly into a vein through an injection or a drip for this.
Things you can do at home:
As well as taking antibiotics for cellulitis, you can help speed up your recovery by:
- Providing paracetamol or ibuprofen for the pain/ fever
- Raising the affected body part on a pillow or chair when you're sitting or lying down, to reduce swelling
- Regularly moving the joint near the affected body part, such as your wrist or ankle, to stop it getting stiff
- Encouraging your child to drink plenty of fluids to avoid dehydration
Not all cases of cellulitis can be prevented but steps can be taken to reduce the risk of developing cellulitis.
You can reduce the risks of developing cellulitis by:
- Encouraging your child to wash the hands regularly
- Lean any cuts or wounds and use antiseptic cream
- If your child has eczema or another skin condition keep their skin clean and well moisturised



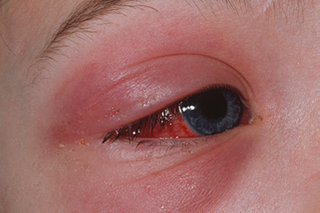 link to cellulitis page
link to cellulitis page